Perimenopause and Menopause Explained
Several factors can influence the timing of Perimenopause and Menopause, including: genetics, overall health, and lifestyle. The age at which women begin Perimenopause and Menopause can vary widely.
Perimenopause – Typically begins in a woman’s late 30s to early 40s, although it can start as early as the mid-30s or as late as the early 50s. Perimenopause is the transitional phase leading up to menopause when hormonal changes and symptoms begin to manifest. It can last anywhere from a few years to over a decade before menopause officially occurs.
Perimenopause characterized by a range of symptoms as a result of fluctuating hormonal levels. These symptoms can vary widely from woman to woman and may include:
- Irregular Menstrual Cycles: One of the hallmark signs of perimenopause is irregular periods. Menstrual cycles may become shorter or longer, and the flow can be heavier or lighter.
- Hot Flashes and Night Sweats: These are common and often the most bothersome symptoms. Hot flashes are sudden feelings of heat that can cause flushing, sweating, and a rapid heartbeat. Night sweats are hot flashes that occur during sleep.
- Sleep Disturbances: Many women experience difficulty sleeping during perimenopause. This can be due to night sweats, anxiety, or other factors.
- Mood Changes: Hormonal fluctuations can lead to mood swings, irritability, and increased susceptibility to stress and anxiety.
- Vaginal Changes: The vaginal lining may become thinner and drier, leading to discomfort during intercourse and an increased risk of urinary tract infections.
- Changes in Libido: Some women experience a decrease in sexual desire during perimenopause, often due to hormonal changes and vaginal discomfort.
- Breast Tenderness: Hormonal fluctuations can lead to breast tenderness and soreness.
- Fatigue: Many women report feeling more tired during perimenopause, which can be influenced by hormonal changes, sleep disturbances, and other factors.
- Headaches: Some women experience more frequent or severe headaches during perimenopause.
- Changes in Hair and Skin: Hair may become drier, thinner, or less lustrous, and the skin may become drier. Acne or changes in skin pigmentation can also occur.
- Weight Gain: Changes in metabolism and hormone levels can lead to weight gain, especially around the abdominal area.
- Memory and Cognitive Changes: Some women report lapses in memory, difficulty concentrating, or “brain fog.”
- Joint and Muscle Aches: Musculoskeletal symptoms like joint pain and muscle stiffness can occur.
It’s important to note that not all women will experience all of these symptoms, and some may experience them to a greater or lesser extent.
Menopause – Is defined as the point in time when a woman has not had a menstrual period for 12 consecutive months. It usually occurs in a woman’s late 40s or early 50s, with the average age of onset in the United States/Australia being around 51. However, the age at which women experience menopause can vary significantly. Some women may go through menopause in their early 40s or as late as their mid-50s.
Menopause comes with a variety of physical and emotional symptoms similar to the ones listed above for Perimenopause, there are a couple of aditional possible changes to be aware of:
- Urinary Changes: Weakened pelvic floor muscles can lead to urinary incontinence or increased urgency to urinate.
- Osteoporosis Risk: The risk of osteoporosis, a condition characterized by reduced bone density and an increased risk of fractures, may increase during and after menopause due to hormonal changes.
What Are The Different Stages of Menopause?
Menopause is a multi-stage process that typically includes several distinct phases:
- Perimenopause: Perimenopause is the transition leading up to menopause. It can begin several years before menopause itself and is characterized by hormonal fluctuations. Women may experience irregular menstrual cycles, hot flashes, and other menopausal symptoms during this phase. Perimenopause can last for several years and often begins in a woman’s late 30s or early 40s, but it can start earlier or later.
- Menopause: Menopause is defined as the point in time when a woman has not had a menstrual period for 12 consecutive months. It typically occurs in a woman’s late 40s to early 50s, with the average age of onset in the United States being around 51. Menopause marks the end of a woman’s reproductive years.
- Postmenopause: Postmenopause is the phase that follows menopause. It encompasses the years after menopause has occurred. During postmenopause, hormonal fluctuations stabilize, and many menopausal symptoms, such as hot flashes, become less severe or may subside altogether. However, postmenopausal women are at an increased risk of certain health conditions, including osteoporosis and heart disease.
- Early Menopause: Some women experience early menopause, which occurs before the age of 40. Early menopause can be due to genetic factors, medical conditions, surgical interventions (e.g., removal of the ovaries), or other factors. The symptoms and health implications of early menopause are generally similar to those of natural menopause.
- Surgical Menopause: Surgical menopause results from the surgical removal of both ovaries (bilateral oophorectomy) before a natural menopause occurs. This can lead to an abrupt onset of menopausal symptoms. Women who undergo surgical menopause are at an increased risk of certain health issues and may need hormone replacement therapy to manage symptoms and reduce health risks.
How Your Hormone Levels Change During Menopause
The production of estrogen and progesterone decreases significantly during menopause, leading to various physical and emotional changes. The extent of this decline can vary among individuals, but here is a general overview of how the production of these hormones decreases during menopause:
ESTROGEN
- Perimenopause: During perimenopause, which typically begins in a woman’s late 30s or early 40s, estrogen levels can fluctuate dramatically. While estrogen production may still occur, it is no longer as consistent as it was during the reproductive years.
- Menopause: As a woman enters menopause, typically in her late 40s or early 50s, estrogen production significantly decreases. In some cases, it can drop to just 40-60% of the levels experienced during the reproductive years.
- Postmenopause: After menopause, estrogen production remains consistently low. The ovaries produce very little estrogen, and the primary source of estrogen becomes adipose (fat) tissue.
PROGESTERONE
- Perimenopause: Similar to estrogen, progesterone production can also fluctuate during perimenopause. It may decline as women enter this transitional phase.
- Menopause: After menopause is reached, the production of progesterone significantly decreases. The ovaries become less active, and ovulation ceases, leading to minimal progesterone secretion.
It’s important to note that individual experiences with hormonal changes during menopause can vary. Some women may have a more abrupt and significant decline in hormone production, leading to more severe symptoms, while others may have a smoother transition. The decrease in estrogen and progesterone levels is responsible for many of the symptoms and health changes associated with menopause, including hot flashes, mood swings, changes in bone density, and increased risk of certain health conditions.
A rencent study (2023) noted Black, Asian, and Latina women on average begin menopause earlier than white women, have longer transition periods, and experience more intense hot flashes and vaginal symptoms.
For women who experience lifestyle limiting symptoms or who are at risk for health issues due to hormonal changes, hormone replacement therapy (HRT) may be recommended by a healthcare provider. HRT involves supplementing estrogen, and sometimes progesterone, often in a in a wearable patch or topically applied gel/cream to help alleviate symptoms and reduce health risks. The decision to use HRT should be made in consultation with a healthcare provider, who can assess individual needs and health risks.
Lifestyle related Breast Cancer Risk Factors to also consider
Drinking alcohol – Is clearly linked to an increased risk of breast cancer. The risk increases with the amount of alcohol consumed. Women who have 1 alcoholic drink a day have a small (about 7% to 10%) increase in risk compared with those who don’t drink, while women who have 2 to 3 drinks a day have about a 20% higher risk. Alcohol is linked to an increased risk of other types of cancer, too.
Being overweight or obese – Before menopause, a woman’s ovaries make most of her estrogen, and fat tissue makes only a small part of the total amount. After menopause (when the ovaries stop making estrogen), most estrogen comes from fat tissue. Having more fat tissue after menopause can raise estrogen levels and increase the chances of getting breast cancer.
Women who are overweight also tend to have higher blood insulin levels. Higher insulin levels have been linked to some cancers, including breast cancer.
Not being physically active – Evidence is growing that regular physical activity reduces breast cancer risk, especially in women past menopause. The main question is how much activity is needed. Some studies have found that even as little as a couple of hours a week might be helpful, although more seems to be better.
Does using HRT increase the risk or brest cancer?
Some females using HRT will be diagnosed with breast cancer slightly more often than those not using HRT. The studies showing this were using non-body-identical HRT in certain groups of females and the risk is very small. There is no increased risk of dying from breast cancer nor any increased risk of dying from any cause (all cause mortality).
It is not clear whether this is caused by the HRT. It may be that the women were examined more often because they were on HRT, or that early cancers grew more quickly.
Studies show that about one extra case of breast cancer in 1000 women is diagnosed when women use combined HRT – oestrogen AND progestogen (non-body-identical formulations of progesterone).
Studies show that women using oestrogen alone (without progesterone) have lower rates of breast cancer diagnosis – also about one less diagnosis in 1000 women.
A pooled statistical analysis of thirty clinical trials found that women who began hormone therapy before age 60 had a 39% lower risk of death than women who didn’t take hormones. Do your research, takinging into account your own family history, you deserve to live a fullfilling life, suffering with menopausal symptoms should not be considered a badge of honour, nor should women be expected to suffer in silence, or suffer becuase our Mothers or Grandmothers did so. We now have acces to medical and scientific advances to imporve our quality of life, we also have the ability to make certain lifestyle choices to imporve our longivity – advocate for YOU!
Personal Recomendation – I can highly recommend watching Channel 4’s (United Kingdom) taboo-smashing documentary, ‘Sex, Myths and Menopause’ with Davina McCall, you can also listen too or read the book ‘Menopausing The Positive Roadmap to Your Second Spring‘ Author Davina McCall.
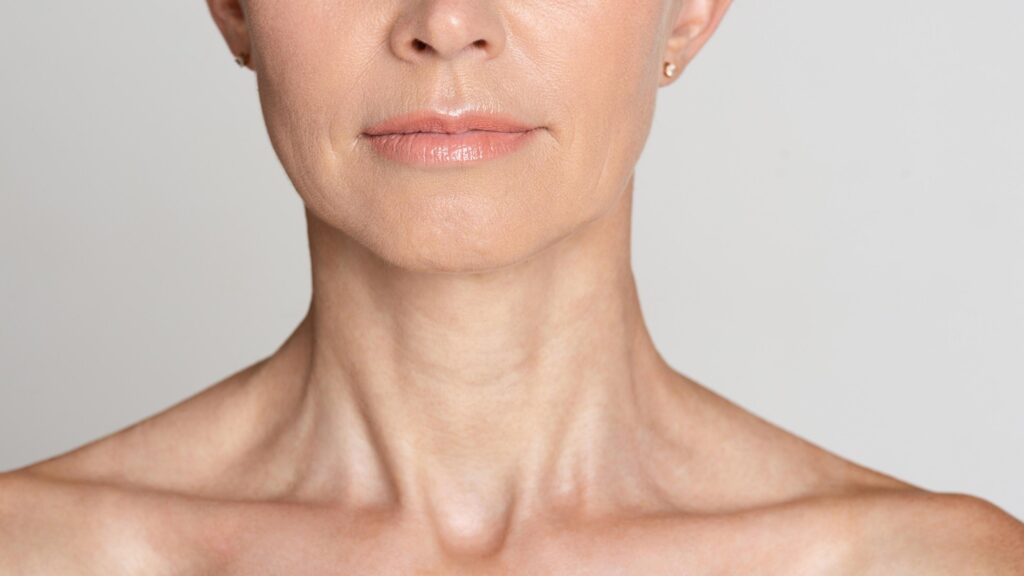
How does your Skin Change during Menopause?
Menopause is a natural biological transition in a woman’s life, signifying the end of her reproductive years. It is typically characterized by a range of hormonal changes, and these hormonal shifts can have a significant impact on the skin. Here are the key ways in which menopause affects the skin:
- Reduced Collagen Production: Estrogen, which declines during menopause, plays a crucial role in maintaining collagen production in the skin. Collagen is responsible for skin’s firmness and elasticity. As estrogen levels drop, collagen production decreases, leading to a loss of skin firmness and the development of wrinkles and fine lines.
- Loss of Skin Elasticity: Elastin, another protein responsible for skin elasticity, also declines during menopause. This contributes to sagging skin, particularly in the neck and jawline.
- Skin Dryness: The skin may become drier during menopause due to decreased oil production. This can lead to itchiness, flakiness, and a feeling of tightness.
- Hyperpigmentation: Melanin synthesis is regulated by estrogen, as estrogen levels reduce so the production of melanin can increase and it is melanin that causes age spots, melasma, and other forms of hyperpigmentation. These dark spots can appear on the face, neck, and hands, these often occur in areas of the body that have been previously exposed to UV rays over the years.
- Acne and Breakouts: Some women experience adult acne during menopause due to hormonal imbalances. Acne often appears on the lower face, chin, and jawline.
- Sensitivity: Menopausal skin can become more sensitive, leading to increased redness, irritation, and the development of conditions such as rosacea.
- Slower Cell Turnover: The skin’s ability to shed dead skin cells and generate new ones may slow down, resulting in a dull complexion and slower healing of blemishes or injuries.
- Thinning Skin: A reduction in skin thickness is common during menopause, making the skin more fragile and susceptible to injury.
- Hormonal Changes: Hormonal fluctuations can affect the skin’s sebaceous glands, potentially leading to changes in oil production and the development of acne or dryness.
It’s important to note that not all women will experience these skin changes to the same extent or in the same way. Genetics, lifestyle, and overall skin care practices can also influence how the skin responds to menopause.

How To Care For Menopausal Skin
To support skin health during perimenopause and/or menopause, consider the following tips:
- Adjust your skincare routine to address the specific needs of your skin during this phase, such as hydration and moisturisation.
- Prioritise sun protection to prevent further damage, as perimenopausal and/or menopause skin may be more sensitive to UV radiation.
- Use products with ingredients that focus on boosting collagen production.
- Maintain a balanced diet rich in antioxidants, omega-3 fatty acids, and vitamins to nourish your skin from the inside out.
Targeted Ingredients for Menopausal Skin Support
Our Multi-Purpose Products are formulated to target multiple skin concerns, below is a quick overview of menopausal skin concerns along with specific cosmetic ingredients in each FIFTY7KIND Product:
LUCA LIPID FERMENT VITAMIN C SERUM:
- Reduced Collagen Production – G.G.P Molecule, Marine Bamboo and Fermented Willow Bark
- Loss Of Skin Elasticity – Marine Bamboo and Astaxanthin
- Skin Dryness – COQ10, Algae Complex, and Sensolene
- Hyperpigmentation – VC-IP (Vitamin C Derivative), COQ10, Fermented Licorice Root, Astaxanthin and Chromabright Molecule
- Acne/Breakouts – Fermented Willow Bark, Regu-Seb, and Fermented Lipids
- Sensitivity – Glass Microalgae, and Essential Oil Free Formulation
- Slower Cell Turnover – Fermented Willow Bark
TANU SKIN AFFINITY COACTIVE SERUM:
- Reduced Collagen Production – Sytenol A, Aroleat Samphira and Fermented Willow Bark
- Loss Of Skin Elasticity – Omegia
- Skin Dryness – Phospholipids
- Hyperpigmentation – Sytenol A
- Acne/Breakouts – Sytenol A, Fermented Willow Bark, and Aroleat Samphira,
- Slower Cell Turnover – Aroleat Samphira and Fermented Willow Bark
NADI INNATE FLOW QUELL BALSAM:
- Reduced Collagen Production – Collageneer
- Loss Of Skin Elasticity – L22, Ceramide NP, and Collageneer
- Skin Dryness – COQ10, L22, Phospholipids, Ceramides, Sterols and Hyaluronic Acid
- Hyperpigmentation – L22
- Sensitivity – Calming Complex
- Thinning Skin – Repair Complex and Ceramide NP
Remember that the effects of perimenopause and/or menopause on skin can vary from person to person, so it’s essential to tailor your skincare routine and lifestyle practices to your individual needs. Please reach out via email for any help/advice: gabrielle@lovefifty7kind.com
Until next time, be human, be kind, be you
REFERENCES:
- Farage, M. A., & Maibach, H. I. (2008). Long-term changes in skin physiology and appearance as related to chronological aging. Contact Dermatitis, 58(5), 234-241.
- Makrantonaki, E., & Zouboulis, C. C. (2007). Molecular mechanisms of skin aging: state of the art. Annals of the New York Academy of Sciences, 1119(1), 40-50.
- Pereira, S. G., & Malaquias, A. R. (2020). Lymphatic system and skin diseases. Clinics in Dermatology, 38(3), 303-309.
- Mortality associated with hormone replacement therapy in younger and older women: a meta-analysis – Database of Abstracts of Reviews of Effects (DARE): Quality-assessed Reviews – NCBI Bookshelfhttps://www.ncbi.nlm.nih.gov/books/NBK70639/
- Does HRT cause breast cancer?
https://vivhealth.com.au/menopause-treatment/does-hrt-cause-breast-cancer-2/ - Reeves AN, Elliott MR, Harlow SD Selection Bias Masks Racial Differences in Age at Menopause: The Study of Women’s Health Across the Nation JAMA Open Network 956MS2
Comments +